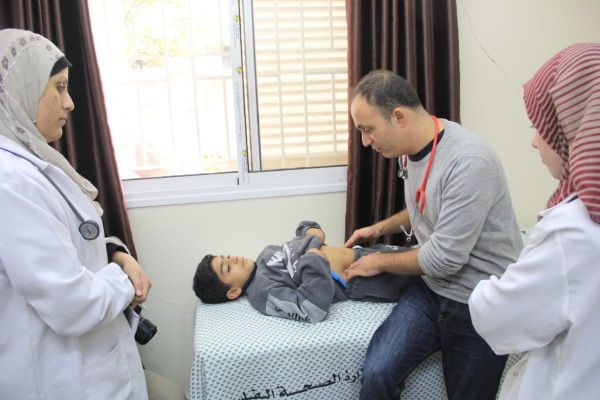
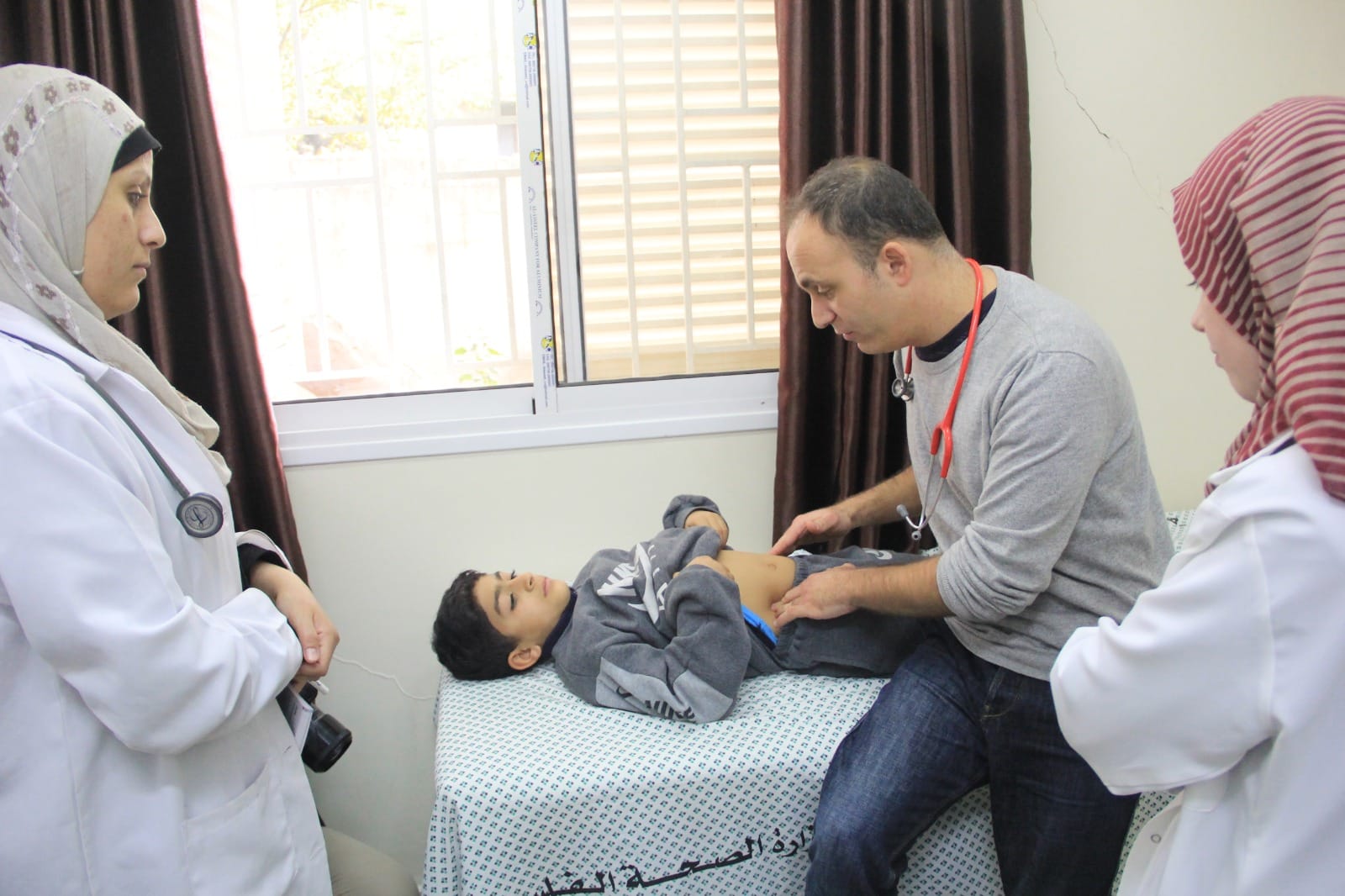
The Dilemmas of Practicing Humanitarian Medicine in Gaza
Humanitarian medical aid was developed to provide life-saving assistance to populations suffering from war and disease. What happens when this model is applied to help those living under occupation and coping with chronic deprivations and long-term siege conditions? Osama Tanous, a Palestinian pedia