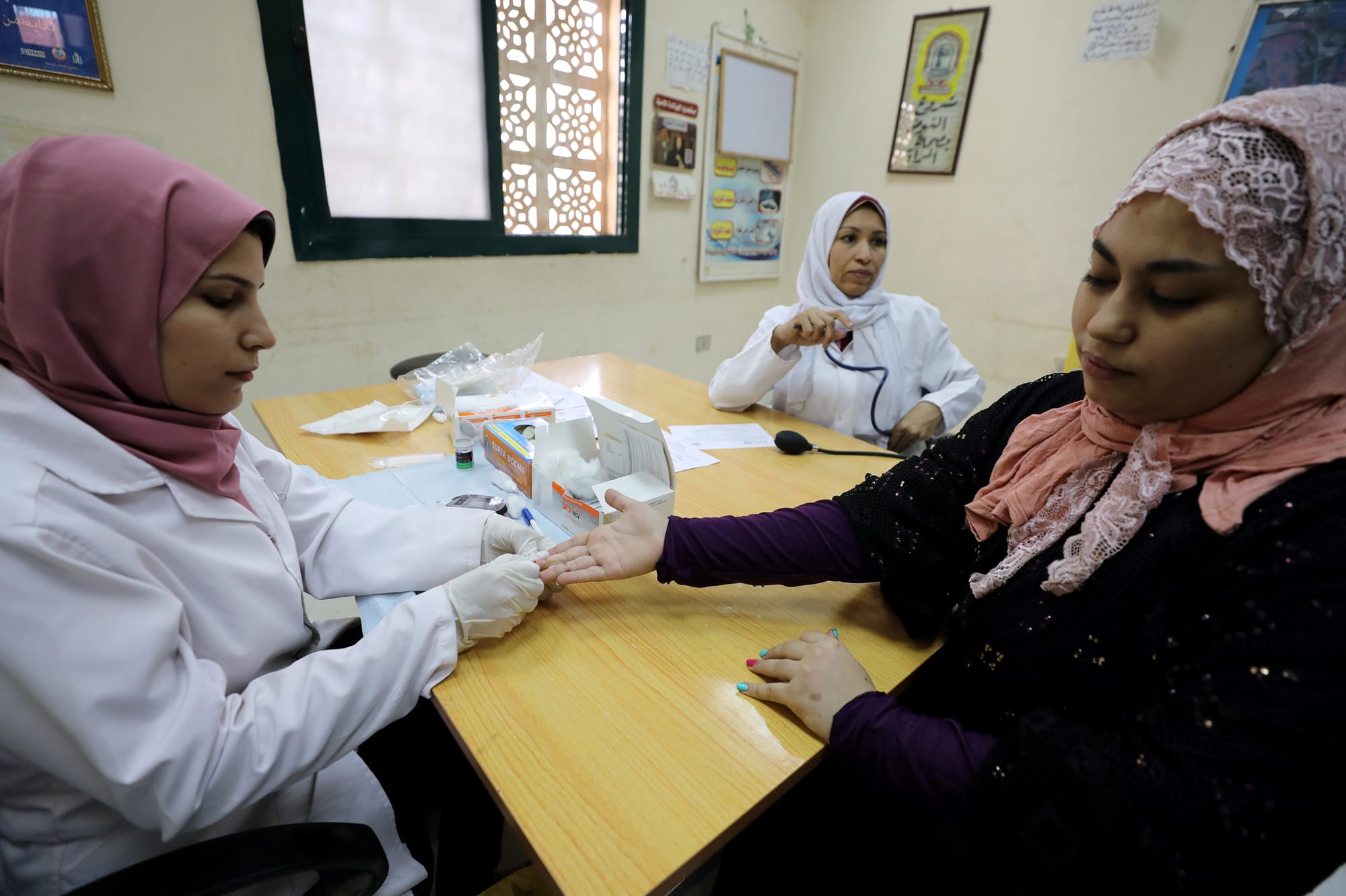
Hepatitis C, COVID-19 and the Egyptian Regime’s Approach to Health Care
As social phenomena, epidemics and the responses they generate reveal much about a country’s political economy and a state’s relationship with its citizens. In Egypt, the manner in which President Abd al-Fattah al-Sisi’s regime has approached an epidemic of hepatitis C on the one hand and the arriva